Abstract
This study sought to examine participants’ experience of attending a Newborn Behavioural Observations (NBO) training and implementing it into community services, within an Irish context. Semi-structured interviews were conducted with participants of the training (n=6, female=100%), while Thematic Analysis (TA) was utilised to analyse qualitative data. Three main themes emerged along with their related subthemes: ) Parallel experience between training experience and application into practise, 2) Deeper understanding of a baby’s capacities and value of a relational approach, and 3) Ruptures and Connections. The findings suggest that participants felt empowered, with an increased level of confidence when working with babies and parents following the training. Future research could usefully focus on accessing a wider range of service providers. While future NBO training might consider the need for ongoing peer support groups to sustain and develop NBO learnings.
Introduction
The quality of the early relationship between parent and infant is crucial for the long-term social, emotional, physical, and cognitive development of children (Alvares, 2014). However, it can be difficult to understand the needs of babies and what they are trying to communicate. The Newborn Behavioural Observations (NBO) System is an interactive, infant-focused, relationship-based tool (Nugent, 2015). The NBO consists of 18 neurobehavioural observations (usually 15-20 minutes), used with infants from birth to 3 months. While few in number, studies exploring practitioner experiences of applying the NBO have yielded positive preliminary results (McManus & Nugent, 2011; Hawthorne & Nicolau, 2017).
Holland and Watkins (2015) researched the use of the NBO by Flying Start (FS), an early year’s programme in Wales. The study used a questionnaire of fixed choice questions, to research health visitors (N=12) view of implementing the NBO. All respondents believed the NBO enhanced parental understanding of their baby’s behaviour and how to meet their baby’s needs; with 75% of respondents indicating that implementation of the NBO helped to build the parent-infant relationship. Furthermore, eleven respondents reported that the NBO helped to build and enhance the therapeutic alliance between parent and practitioner. However, the study highlighted barriers such as language, when time was short, when a particular family’s home environment was chaotic or the family was in crisis, or when the birth was a multiple one, and the need to develop an NBO champion role within the locality in order to facilitate the sustainability of the NBO.
Kristensen et al. (2019) study utilised a cluster randomised design to compare 56 Danish health visitors who had completed NBO training, with 55 who had not. They found significant differences with regard to knowledge about infant self-regulation between the two groups. Significant differences were not observed on the other competencies measured (intention, self-efficacy, and observation skills). However, generalisability of the results beyond Denmark remains to be seen.
Kristensen and colleagues’ (2019) results are broadly consistent with the findings of Hawthorne and Nicolau (2017) who surveyed the use of the NBO by practitioners (N=133), approximately seven months after the NBO training course in the UK. The cross-sectional study was made up of a variety of professionals. The study found that practitioners were using the tool in a flexible manner; some were using it as a whole routinely, while others were using just parts of it. 84% of practitioners reported carrying it out with both fathers and mothers. Overall, the study found that the training had a positive impact on upskilling practitioners working in infant and perinatal mental health. The study highlighted the need for more practice in order to become proficient using the tool and the need for continued professional development.
In 2011, McManus and Nugent compared the experiences of two groups of practitioners working with ‘high risk’ newborns and their families who were engaged with early intervention service providers in the United States. One group provided usual care, while the NBO was utilised with the other group. The group of early intervention providers who were in the NBO group reported higher perceived confidence working with high-risk newborns than those who provided usual care.
Appleton, Nickell, and Nicolau (2016) in their unpublished study compared three groups of Health Visitors from NBO training courses according to preparation prearranged by their facilitator. Results of the study found that the NBO training can be more effective for practitioners with a strong background in infant mental health, but short training preparation can also be beneficial. This has important implications for the preparation of practitioners ahead of NBO trainings.
No other known study has examined the experiences of practitioners training in and applying the NBO within an Irish context. It is hoped that upon completion of the study an enhanced understanding of the experiences of practitioners applying the NBO, within an Irish context, will be obtained and inform future training needs.
Procedure
The Tipperary Infant Mental Health Steering Group (TIMHSG) hosted specialist training in the NBO. The training was provided by the Brazelton Centre UK and was attended by 26 practitioners. A convenience sample was utilized to complete the semi-structured interview. All 26 participants who attended the training, were invited to self-select and ‘opt in’ to the study, by contacting the researchers by email. In total, six practitioners consented to participate in the study. Participants were female (100% and worked across a range of community services.
For the purpose of this study, Thematic Analysis (TA) was utilised to analyse qualitative data, as it also offers a flexible, inductive and exploratory approach that fits with the aims of the research (Braun & Clark, 2006). Issues in relation to research reflexivity were addressed and considered throughout the analysis process.
Results
Three main themes emerged. These were (1) Parallel experiences between NBO training and application into practise, (2) A deeper understanding of a baby’s capacity and value of a relational approach, and (3) Ruptures and connection. These are defined below along with their related subthemes, which are supported by illustrative quotes. After each quote, “Ppt” indicates a participant number in order to protect the anonymity of the participants. Table 1 illustrates the Primary Themes and Subthemes identified in the qualitative analysis.
Table 1. Themes and Subthemes.
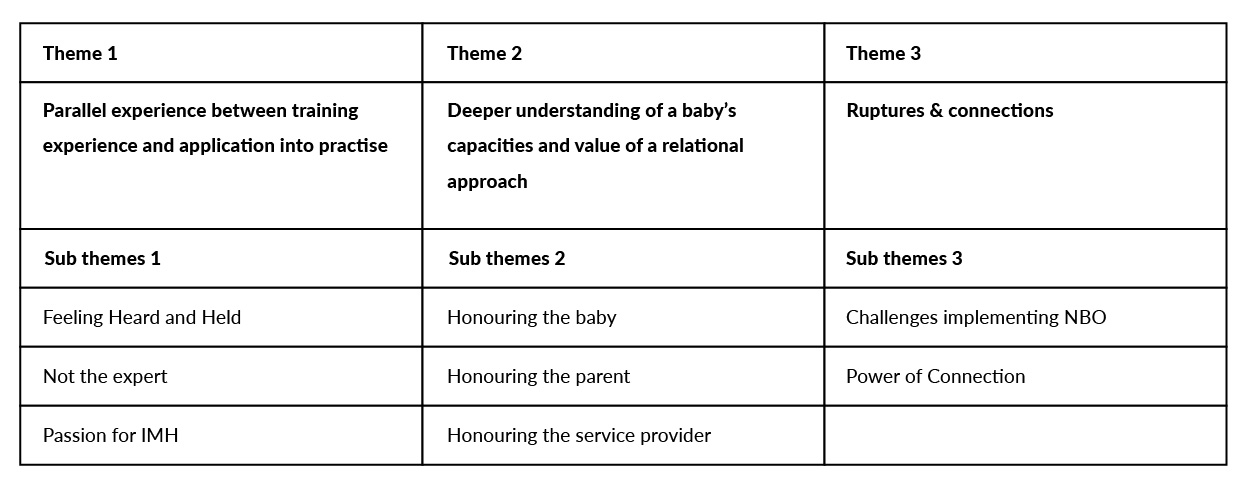
Theme 1: Parallel experience between NBO training and application into practise. Parallel experience refers to the participant’s experiential experience attending the training and applying the same key experiences into their work with babies and parents; experiences such as collaboration, respect, non-judgmental, supportive, and enthusiasm. It also referred to the teaching methods and how they were experienced and in turn how participants integrated the NBO into their respective services. This theme transpired in the following subthemes.
1.1 The experience of being heard was reported by most participants and it described a deep sense of feeling listened to, and validated during the training, which left a lasting impression, as one participant noted “Everyone was listened to, you could see if you asked a question, you really felt listened to, very comfortable to ask questions that you thought were silly, or obvious or something you should have known it was a lovely, lovely training” (Ppt 4). Similarly, in turn, participants spoke about using the NBO to really listen to, and give voice to the baby, as one participant reflected “You are going in to be with that baby and if you see the baby is crying then you are making an observation and you are wondering well, I wonder if she is a bit over stimulated. Saying things from the babies perspective” (Ppt 3).
Participants reported feeling ‘held’ by the concrete teaching methods pre and post-training. One participant commented, “what I really liked is that you got sent stuff (NBO materials) beforehand, so it was not all cramped into one day. I remember we watched those presentations that the trainer had done, that was good to get you into the space beforehand, so that was very helpful, so it wasn’t overburdening you on the day” (Ppt 1).
1.2 Not the expert referred to participants experience of observing the trainer adopting a non-expert stance when interacting with the parent and infant, during the training, as one participant commented, “I remember her (trainer) first asking the mam what she noticed about the baby, actually what she learnt about the baby so far, so even from the beginning having that sense of we don’t have all the answers, you have answers on your baby and your baby will show us” (Ppt 1). This experience was mirrored by practitioners when they applied this experience in their practise, as one participant reflected “We are not the experts we are the learners. We are not going in as an expert and saying, “Let’s see if your baby can do ABC, we are working with the parent and with the baby and we are learning with the Mom, so it is good in that sense” (Ppt 4).
1.3 Passion for Infant Mental Health (IMH) refers to the participant’s experience of the trainer’s passion for the NBO and IMH work, which resulted in a renewed sense of enthusiasm and passion in the participants work with infants. One participant reflected, “it was their personalities too, of the people that delivered the training and their passion, I think it was their passion that came through so well” (Ppt3). With one participant commenting that the passion she experienced both at the training and applying the NBO was the “missing link” for her (Ppt 3).
Theme 2: Deeper understanding of a baby’s capacities and the value of relational approach with parents. It comprised of three subthemes which focused on the uniqueness of each baby, the therapeutic alliance with the parent and the effect of the training on the service provider.
2.1 Honouring the baby referred to participants appreciating the unique capacity of each infant, and using the tool as one participant noted, to wonder and begin to explore alongside the parent, “who is this baby? Who is this little one? What’s the little character here? We are talking about the little person in there. We are not talking about what the two-month-old should be doing, we are talking about who is the little person in there, who is the little character, what is the temperament, how unique they are” (Ppt 4).
2.2 Honouring parent referred to participant’s experience of implementing the NBO in order to establish a relationship, as one participant described, “it (NBO) really helps with the relationship with the parent, and sometimes it (NBO) can be the building stone for the relationship” (Ppt 5). Honouring the caregivers also referred to meeting the parent where they are at, and being mindful of same as one, participant noted, “for the mom then that has so much else going on, you are really looking and trying to indirectly say ‘oh your baby is yawning or he is looking away, or does he always jump in his sleep” (Ppt 3).
2.3 Honouring the service provider this was reflected in how the participants experienced their value as service providers as one participant noted, “I wouldn’t be academic but I would be confident that I can read a baby and the NBO has been so instrumental in that for me. It really opened up a whole way of working for me” (Ppt 4). While one participant reflected that she felt “more reassured when you are pointing something out, you have something to back up what you are saying” (Ppt 6).
Theme 3: Ruptures and Connecting. Ruptures referred to barriers for participants in their attempts to integrate the NBO into their services. Connecting was a parallel theme that referred to participants renewed values on the power of connections when faced with ruptures. This theme transpired in the following subthemes: (3.1) Obstacles implementing NBO and (3.2) The Power of connecting
3.1 Obstacles implementing NBO refers to the two main obstacles reported by participants when trying to implement the tool; not having regular access to babies between 0-3 months and the COVID-19 pandemic. One participant noted, as her service works with a broad range of ages (0-18 years) she had difficulty accessing babies under 3 months, “I actually didn’t do any NBO unfortunately. I didn’t have anybody with that age bracket” (Ppt 2). Participants who had access to babies noted that doing it over zoom was an obstacle with one participant reporting, “never really, because the baby is rarely ready at that time and the mom is concentrating on the baby and it just doesn’t seem to work” (Ppt 4).
3.2 Connection refers to linking in with other service providers, with parents and babies, and this theme emerged throughout all the interviews as one of importance. One participant reflected on the post-training video group meetings, “For me, it meant when I was doing the NBO I’d have questions, and then I could bring them to the group and then I could hear other people’s questions so that was really helpful” (Ppt 1). Video calls were also used by some participants with babies and their parents as a way of helping them stay connected. One participant reflected, “It’s very difficult. Even to do it on zoom. But what I do is talk the mom through it. Talk to parent about how the baby is doing” (Ppt 4). Post-training supports via group Zoom calls were also noted as a great support to keep the interest and motivation alive as one participant reflected, “being linked in with Boston and what they have to offer in terms of the lectures and training is really, really important” (Ppt 3).
Discussion
This is the first Irish study to explore participant’s experience of attending an NBO training and integrating it into services. The present study allows us to understand the perspectives of participants experience attending the NBO training, how it informed their practice and how they applied it to their work.
The findings in this study provide a lens to understand the power of relationships. Theme 1 “Parallel Experience” described how the experience of receiving the training and how it was delivered was equally as important as the NBO teaching tool in and of itself. Captured in three subthemes the ‘parallel’ speaks to the participant’s experience of the trainers, the training, and the same experience shared between participants and the families they work with. This theme illustrated the participant’s emotional reaction to the trainers, the pace and organization. Holland and Watkins (2015) research also referenced relationship themes in so far as they found that respondents believed the NBO enhanced parental understanding of their baby’s behaviour, built the parent infant relationship and helped build relationships between the practitioner and parent.
The present study also illustrated the participant’s deeper understanding of a baby’s capacity, the importance of observing the baby, and honouring the parents as experts of their baby. Participants particularly identified their increased confidence working with babies and how the NBO was an extra tool they have to back up existing IMH informed service delivery and this seemed particularly important given the challenges faced during COVID-19. This is broadly consistent with Hawthorne and Nicolau’s (2017) study which found that the NBO training had a positive impact on upskilling practitioners. Findings by McManus and Nugent (2011) also reported higher perceived confidence working with high-risk newborns than those who provided usual care.
Similar to other research studies (Holland & Watkins, 2015), challenges were identified with integrating the NBO into services. In particular, we learned that not all participants were able to apply the NBO as they did not have access to babies within their services. This has important implications for service providers and practitioners ahead of NBO trainings. Holland and Watkins (2015) in their study also highlighted the need to develop an NBO champion role. Similarly, we learn in this study the importance of connecting with other service providers and the need for ongoing peer support groups to sustain and develop NBO learnings.
A strength of the present study is its qualitative design which allowed access to the personal reflections of participants and their insights, which will be helpful for future training, particularly within an Irish context. There is a limitation in basing views of an NBO training for participants, where there is a small sample size. Future research could use a longitudinal research design, focusing on the medium to long terms impact of the training to determine whether participant’s reflections are sustained and integrated after an extended period of time.
References
Alvares, M. A. (2014). The baby as a person not as a patient: Using the NBO in Paediartic Primary Care in an Urban Spanish Setting presented at the World Congress of WAIMH, Edinburgh, 2014. (Unpublished)
Appleton, J., Nickell, I., & Nicolau, S. (2016). Evaluating the impact of preparation for health visitors prior to attending the NBO training on later use with families, presented the results at the 15th World Congress of WAIMH, Prague, June 2016. (Unpublished)
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3, 77–101.
Nugent, J. K., Bartlett, J. D., Von Ende, A., & Valim, C. (2017). The Effects of the Newborn Behavioural Observations (NBO) System on Sensitivity in Mother-Infant Interactions. Infants & Young Children, 30(4), 257-268.
Hawthorne, J., & Nicolau, S. (2017). Newborn Behavioural Observations System: Benefits and opportunities for integration into practice. Journal of Health Visiting, 5(7), 352-357.
Holland, A., & Watkins, D. (2015). Flying Start health visitor’s views on implementing the Newborn Behavioral Observation: barriers and facilitating factors. Community Practitioner, 88(6), 33-36.
Kristensen, I. H., Vinter, M., Nickell, R. N., & Kronborg, H. (2019). Health visitors’ competences before and after implementing the newborn behavioral observations (NBO) system in a community setting: A cluster randomised study. Public Health Nursing, 36, 856-862.
McManus, B. M., & Nugent, J. K. (2011). Feasibility study of early intervention provider confidence following a neurobehavioral intervention for high risk newborns. Journal of Reproductive and Infant Psychology, 29(4), 395-403.
Authors
Rosarii O’D.Connorton
Dr Aine Herlihy
Ruth Cleary
Correspondence address: Rosarii O’D. Connorton, Primary Care Psychology Service, Western Road, Clonmel, Co. Tipperary, Ireland. Email: Rosarii.ODonnellConnorton@hse.ie








